Nature Medicine - AI Section⭐Exploratory3 min read
Key Takeaway:
Researchers identify five principles to improve precision medicine, aiming for treatments that are effective, reproducible, widely applicable, and fair to all patients.
Coral et al. conducted a study to establish five foundational principles aimed at enhancing the implementation of evidence-based precision medicine, with the key finding being the promotion of clinically meaningful, reproducible, scalable, and equitable health outcomes. This research is significant in the context of healthcare as precision medicine seeks to tailor medical treatment to individual characteristics, thereby improving patient outcomes and optimizing resource allocation. The study addresses the need for a structured framework to guide the integration of precision medicine into clinical practice.
The methodology involved a comprehensive review of current precision medicine practices and the identification of challenges that impede their effective implementation. The authors utilized a multidisciplinary approach, incorporating insights from clinical trials, genomic research, and healthcare policy analysis to propose their framework.
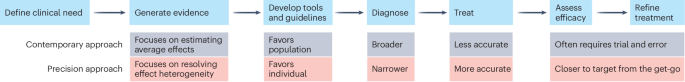
The study identified five tenets critical to advancing precision medicine: clinical utility, reproducibility, scalability, equity, and ethical considerations. The authors emphasize that clinical utility must be demonstrated through robust evidence showing improved patient outcomes, while reproducibility requires that findings be consistently replicable across diverse populations and settings. Scalability pertains to the ability to implement precision medicine strategies broadly across healthcare systems. Equity ensures that advancements in precision medicine benefit all population groups, addressing disparities in healthcare access and outcomes. Lastly, ethical considerations involve safeguarding patient privacy and ensuring informed consent in the use of personal health data.
This approach is innovative as it provides a comprehensive and structured framework that addresses both scientific and ethical dimensions of precision medicine, which have often been considered separately in previous studies. However, the study's limitations include its reliance on existing literature, which may not capture the latest developments in rapidly evolving fields such as genomics and artificial intelligence.
Future directions for this research involve the validation of these tenets through clinical trials and the development of policy guidelines to facilitate the integration of precision medicine into standard care practices. This would require collaboration between researchers, clinicians, and policymakers to ensure effective implementation.
For Clinicians:
"Conceptual study. No sample size. Emphasizes reproducibility, scalability, equity in precision medicine. Lacks empirical validation. Caution: Await further studies for clinical applicability. Consider principles for future research framework."
For Everyone Else:
"Exciting research in precision medicine, but it's still early. It may take years before it's available in clinics. Continue with your current care plan and discuss any questions with your doctor."
Citation:
Nature Medicine - AI Section, 2026. DOI: s41591-026-04309-6 Read article →